The Medicare Sky Is Falling (Part 2)
by run75441
The Medicare Sky Is Falling (Part 2)

Chicken Little, Courtesy of “EW.Com Entertainment Weekly”
Over at The Health Beat Blog, Maggie Mahar explains why the collapse of Medicare HI is less likely with the passage of healthcare reform. The Medicare “Crisis: A Shaggy Wolf Story.
Potentially heading off the shortfall of Medicare funding is the passage of the ACA which is used by the Trustees to forecast a positive projection to Medicare. Before healthcare reform, Medicare HI would run short of funds in 2016. After its passage, the Medicare Trustees forecasted Medicare HI funding lasting to 2024 if Healthcare Reform program implemented. Why is such a delay in insolvency possible? Elmendorf’s (the same Elmendorf who helped kill Hillary-Care) Congressional Budget Office forecasted a $950 billion generated over the next decade from the passage of healthcare reform. Two areas account for most of the savings and the third area could not be measured:
Medicare will be shaving annual increases in payments to hospitals, skilled nursing facilities, home health agencies and other institutions by 1 percent a year for 10 years. The legislation explicitly exempts doctors, calling for reductions ‘in payment updates for most Medical goods and services other than physicians’ services.’ The CBO estimates that this provision will save $196 billion.
Secondly, the ACA raises another $750 billion, primarily by collecting new fees from the health care industry (which can afford the fees because it will have so many new customers); cutting overpayments to private insurers that are not delivering value for Medicare dollars; raising Medicare taxes for those at the very top of the income ladder; and reducing subsidies to hospitals that will no longer be absorbing the cost of caring for 32 million uninsured.
Additionally, The Affordable Care Act paves the way for Medicare to cut spending further, by proposing deep structural reforms that could, ‘transform’ U.S. health care ‘in both the way that it is delivered and the manner in which it is financed.’ The legislation ‘takes important steps in this direction by initiating programs of research into innovative payment and service delivery models,’ the Trustees explain ‘such as accountable care organizations, patient-centered ‘medical homes,’ improvement in care coordination for individuals with multiple chronic health conditions, improvement in coordination of post-acute care, payment bundling, ‘pay for performance,’ and assistance for individuals in making informed health choices.
It is the third point which was not included in Elmendorf’s projection of savings. By overhauling the healthcare delivery model, the Affordable Care Act through Medicare will reduce the healthcare industry cost inflationary cycle by changing how healthcare is delivered to patients and directly impacting the fees paid today. Instead of rewarding for volume of services delivered, the approach is to reward for value “by encouraging integrated, coordinated care that leads to better outcomes at a lower price. These are unprecedented reforms that have never been tried on a national scale (but have been implemented by the VA) which the CBO did not try to estimate just how much these structural reforms might save. As often is the case, over the long term what cannot be counted may count the most. Note that money saved from this change in services rendered will be above and beyond the $950 billion the CBO did score. These are dollars that could be used to cover the 2024 shortfall.”
Without such a change in the delivery of healthcare, the cost spiral will continue. In Phillip Longman’s “The Best Care Anywhere,” the success achieved in healthcare delivery at the VA has not been rivaled anywhere in the private sector. In a fee for services scenario, the change does come at a loss of profitability when the switch is made to one based on better outcomes at lower costs. Phillips gives one hospital’s experiment in the private sector with integrating quality into its healthcare delivery:
Indeed, any health-care provider in the private sector that holds itself out as providing high-quality care for chronic conditions risks financial ruin. That’s a lesson Beth Israel Medical Center in Manhattan learned after it opened a new diabetic center in March 1999. To publicize the new venture, Beth Israel convinced a former Miss America, Nicole Johnson Baker, herself a diabetic, to pose for promotional pictures wearing her insulin pump. She also posed next to a man dressed as a giant foot, a dark reminder of how poorly managed diabetes often leads to amputation.
To avoid amputation and other dire outcomes, such as blindness and renal failure, the new center adopted a model of diabetic care that rivaled the VA’s in its quality. Highly coordinated teams taught patients how to check their blood sugar levels, count calories, and find the discipline to exercise, all while undergoing prolonged and careful monitoring. Within months, the center succeeded in getting the blood sugar levels of 60 percent of its patients under control — a stunning result that brought it national attention.
But the idealists who conceived this program forgot the business they were in. Health insurers would pay only piddling amounts to cover the cost of a diabetic patient seeing a podiatrist, for example, though such care is essential to reducing the risk of amputation. And insurers would pay even less same time, as word of the center’s excellence in diabetic care spread, patient volume increased by 20 percent a month. Soon the center was running a large deficit, and Beth Israel administrators felt compelled to shut it down. Between 1999 and 2006, three similar centers in New York folded based on the same model of care, and for the same reason. Quality doesn’t pay.
Any change in today’s healthcare delivery reducing the patient/client base and their need for medical services takes from the bottom line. The ACA under Medicare’s tutelage takes on fee for services directly and looks to change it to greater quality and better outcomes. If anything, the experiment at Beth Israel was successful for the patient/client base.
Maggie goes on to pick apart the arguments of the doomsday predictors and naysayers. Holding payment adjustments to a 2% yearly increase over a decade, Medicare will bank on expected productivity gains at hospitals, skilled nursing care facilities, etc. Comments of withdrawal from Medicare by providers and doctors are hollow threats (as doctors are exempted) as > than 50% of hospital revenue comes from Medicare. What hospital is going to withdraw? But, what types of productivity gains are implied?
Having supplies and equipment available on demand at the point of usage for nurses. If this does not sound like making CNC tools resident to the Cell, I don’t know what does. This cuts down on wasted movement.
· Proper inventory control to prevent the over buying of equipment by hospitals. One example cited a $20 million purchase of smart heart pumps over time because the inventory could not be found. Sounds familiar to industry also.
· By having accurate inventories and supplies at the point of usage, a nurse’s time is freed up from looking for supplies that are lost or missed placed and farther away from the patient. In the end a nurse’s time is spent as direct labor in delivering a product to the customer rather than Overhead and indirect labor.
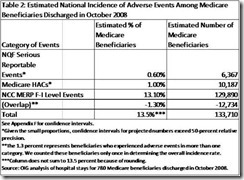
· Fixing the mistakes and errors (most are preventable) being made in hospitals today through error proofing. An Office of the Inspector General, Department of Health and Human Services study found 1 in 7 Medicare patients suffer at least 1 adverse effect from hospitalization. This equates to 1.6 million per year and of that number ~180,000 die. The checklists used by pilots today before take- off could help hospitals and staff lower the incidence of mistakes in hospitals. http://oig.hhs.gov/oei/reports/oei-06-09-00090.pdf “Adverse Events in Hospitals: National Incidence Amongst Medicare Beneficiaries”
Each of these productivity gains has an impact on the costs of operation within a hospital, a direct impact on the quality of the product rendered, and ultimately reducing the amount of time spent in the hospital. While a large part of medical expense is Labor, another part is the ineffective use of resource, assets, and inventory. Looking for the root causes in the end Medicare costs decrease as hospitals become more efficient.
(Rdan…formatting corrections made 6/17)